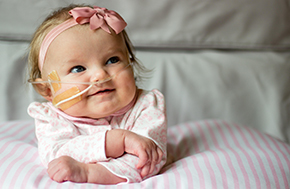
Hope for Lydia Texas Children's
Amy and Joe Krese wanted their two-year-old son to be a big brother. After three miscarriages, their dream was finally coming true. Amy was pregnant with a baby girl, Lydia.
Amy and Joe Krese wanted their two-year-old son to be a big brother. After three miscarriages, their dream was finally coming true.
Amy was pregnant with a baby girl, Lydia.
She’d made it to her 20-week ultrasound scan. “We thought the fear for this pregnancy was behind us,” Amy remembers. But the scan revealed that Lydia had a bilateral congenital diaphragmatic hernia in the muscle separating her chest and abdomen.
Lydia’s abdominal organs had moved upward and crowded her chest. Her lungs were just two tiny slivers on the ultrasound screen and had no room to grow and develop. Instead of preparing to welcome their baby at her birth, Amy and Joe prepared to say goodbye.
“No matter what the outcome was going to be, we had a lot of comfort in knowing that she was in the best hands possible at Texas Children’s. We felt like we had the best counsel from doctors and the best support system -- and if there was something that was worth trying, we would find it there,” recalls Amy.
Then it happened…one month after Amy had gotten Lydia’s devastating diagnosis, she got the call she hadn’t dared to let herself hope for. Her doctors at Texas Children’s had found a possibility.
There was an experimental procedure called fetal endoscopic tracheal occlusion. A balloon would be inserted into Lydia’s trachea, while she was still in utero, preventing the fluid produced by her developing lungs from escaping. The trapped fluid would stretch the lungs, stimulating growth.
It wasn’t a guarantee and it wasn’t a cure, and if Lydia survived beyond the delivery room, she would still need life support and surgery. But it was hope -- the kind of groundbreaking hope that isn’t possible at most other hospitals.
It’s this sort of hope that makes Texas Children’s so unique. Lydia had a chance. And for Amy and Joe, that was everything.
The procedure worked. Her lungs grew. After six weeks, doctors removed the balloon in January 2017. Her mother held her briefly while a doctor took a few photos, and then she was intubated.
Moments like these made Amy’s time at Texas Children’s feel positive, despite the fear and worry. Everyone was “so honest with us from the very beginning, supportive of what we wanted to do… including us in decisions, being positive, but also very realistic,” she says.
Lydia had surgery three days later to repair her diaphragm and spent 80 days in the neonatal intensive care unit (NICU). Then, holding back tears, Amy and Joe said goodbye -- not to Lydia, but to the NICU team that helped save her. Lydia still needed oxygen and a feeding tube, but she could go home.
“The hours of research, the equipment, the time and money -- and the investment in this one experimental procedure -- is not something you think about until it’s your loved one,” said Amy. “My hope is that all families and all kids have the same access to such great care.”
Today, Lydia is 15 months old. She’s in occupational, physical, developmental, and feeding therapy and is quickly catching up with others her age.”